Date:
You know we provide 24-hour emergency and critical care to pets, as well as comprehensive specialty care, but did you know we are the only Veterinary Emergency and Critical Care Society (VECCS) Level 1 Certified Veterinary Hospital in South Carolina?!
The certification program designates three levels (I through III) based on operating hours, equipment ande personnel. Level I is the highest certification level, and the emergency and critical care facilitty must have the resources and specialty training necessary to provide sophisticated and comprehensive emergent and critical care.
The hospital must be open to receive small animal emergency patients 24 hours a day, 365 days a year, and is required to have a board-certified critical care specialist on staff full-time and available for consultation 24/7. Maintaining this level of care is part of our commitment to medical excellence for you and your pets.
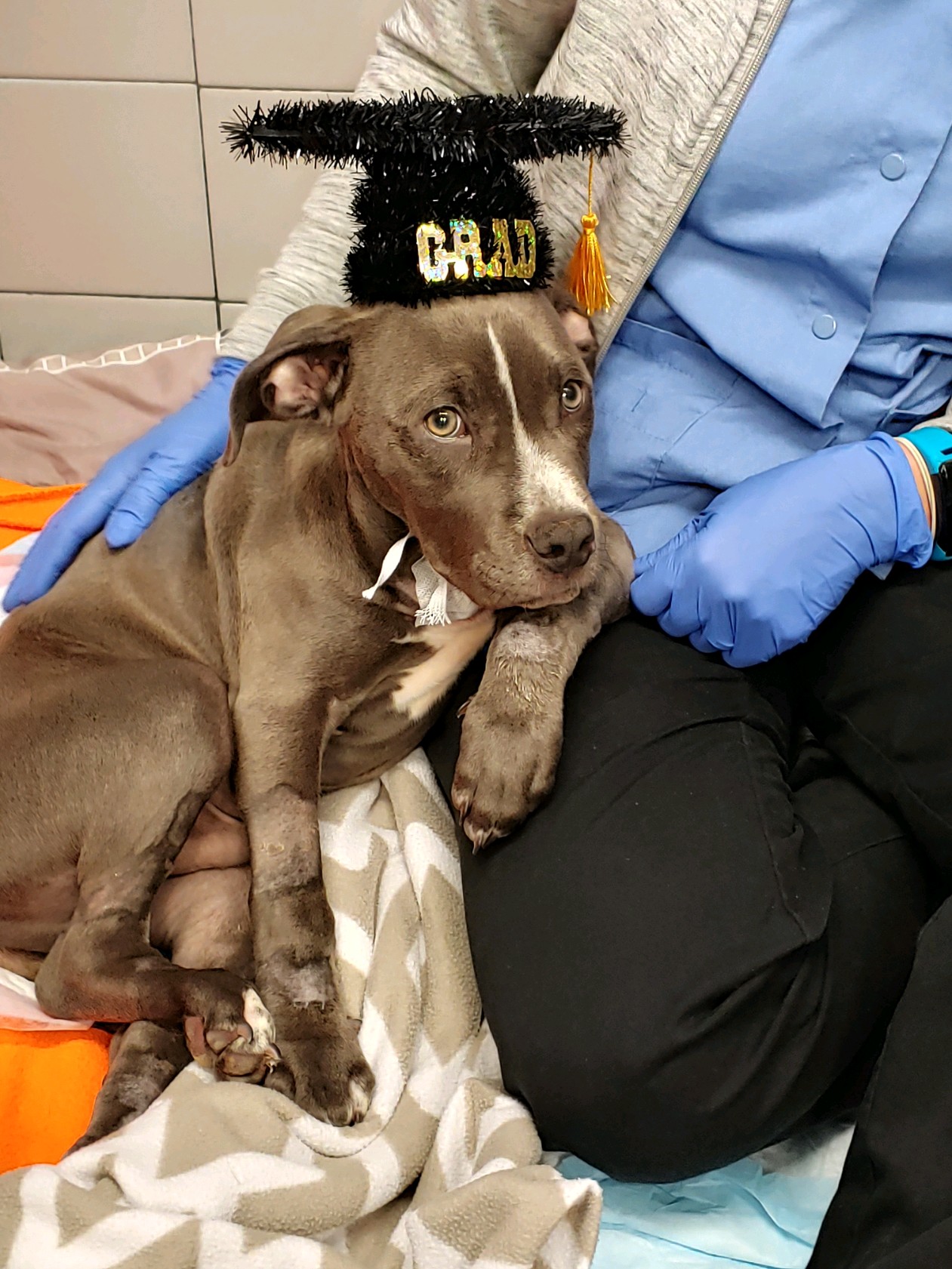
To show you the difference that being a VECCS Level 1 facility makes, we’d like to share the story of Brees, a 14-week old pit bull puppy who suffered a terrible accident and came to our emergency department in May. Brees is a sweet 14-week-old pit bull puppy who came through our emergency department at the beginning of May. His poor mom witnessed him getting hit by a car and she rushed him right over to us.
As a result of the accident, Brees developed severe difficulty breathing and was bleeding from his mouth. X-rays showed a mild pneumothorax (free air in the chest) and severe pulmonary contusions (bruised lungs). Despite supportive care with pain medicine, oxygen therapy, and chest tube placement (to address the pneumothorax), Brees continued to have significant difficulty breathing. Due to concerns about Brees going into respiratory arrest secondary to respiratory fatigue, mechanical ventilation was considered the only option. He was transferred internally to our board certified critical care specialists at this time. Brees was anesthetized, had a breathing tube inserted, and large volumes of bloody or blood-tinged fluid were suctioned from his airways. He was placed on our critical care ventilator and mechanically ventilated (known as "life support" in people). Arterial blood gas monitoring (assessing the levels of oxygen, carbon dioxide, pH, etc.) confirmed acute respiratory distress syndrome (ARDS). ARDS is a potentially life-threatening condition where there are low oxygen blood levels in the body, inadequately supplying oxygen to organs and body systems. Brees required two blood transfusions due to blood loss (primarily into his lungs) and canine albumin transfusions for persistent low albumin (protein).
While on the ventilator, he developed evidence of sepsis (low white blood cell count and low blood pressure). This was suspected to be related to ventilator-associated pneumonia, which is one of the most common complications of mechanical ventilation. Brees required multiple blood pressure stabilizing medications, antibiotic therapy, and systemic support, and fortunately, he eventually stabilized.
After four days of mechanical ventilation, Brees began to improve! A temporary tracheostomy (breathing hole in the neck) was placed to enable weaning from sedatives, and allow him to attempt to breathe on his own. Mechanical ventilation was discontinued, and Brees’s breathing tube was removed on day five. As he remained very weak at this time, we began treating him with physical therapy and acupuncture. He continued to improve and oxygen therapy was discontinued on the seventh day.
Brees began eating, drinking, and walking on his own (despite an injured hip and shoulder blade suffered during the original injury); Brees will have his hip injury addressed in the coming weeks/months as he continues to recover. He was discharged to his owners on day 8 and has continued to improve at home.
As a result of the quick action taken by his family to get him to our hospital, along with our comprehensive emergency and specialty care, highly trained medical team, and advanced technologies - not to mention Brees’ strong will and fighting spirit - he is alive today as an example of what is possible when love, medicine, and an incredibly dedicated team and pet owner come together.
We have now seen Brees for several weekly follow up visits and he continues to improve, grow, and most of all enjoy life with his amazing pet parents!